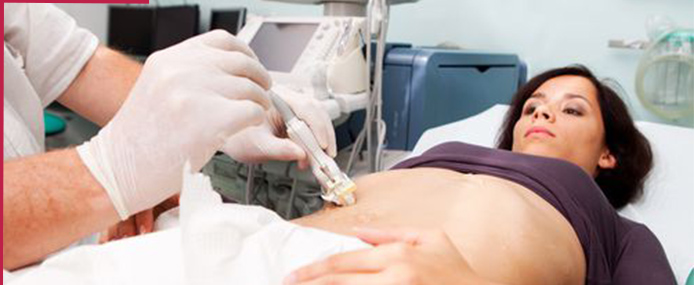
Computed tomography-guided Fine Needle Aspiration Cytology (CT guided FNAC) is a pinhole non-invasive diagnostic procedure done to extract cells from the target site and study them under the microscope for validation and diagnosis. Cells from target sites (eg. breast, skin or any soft tissue) are extracted with the use of a fine needle/syringe, which is inserted through the skin under the guidance of CT so that the margin of error is minimised.

This is a procedure performed by a radiologist to obtain a small tissue sample through a needle. This is done to make a diagnosis and plan future management. CT scan is used to guide the needle into the lesion in the safest possible manner. This is a minimally invasive procedure and is an alternative to an open surgical biopsy. CT guidance generally results in fewer complications, a faster recovery time, and avoidance of general anesthesia.
A definite diagnosis of cancer is almost always based on the histological examination of cell or tissue samples. The procedure used to obtain a specimen for this testing is called a biopsy. Biopsies can be performed by surgical removal of the specimen if the suspicious area is located near the surface of the body or during surgery. If, however, the suspected tumor is located deep inside the body and cannot be seen or felt by the physician, he may decide to perform a CT-guided biopsy. The main advantage of a CT-guided biopsy is that it does not require an incision, but the disadvantage is that in some cases, the needle may not be able to remove enough tissue for analysis.

Percutaneous transhepatic biliary drainage (PTBD) is a common and effective procedure for the palliation of cholestasis in both malignant and benign biliary obstruction, especially after the application of the B-mode ultrasonography guidance . Success rates for PTBD have been reported at 90% or more, and complication rates have been reported at 3% or less .
However, when applied to patients with a special condition (for example, a nondilated bile duct, patient status post left hepatic lobe resection, patient status post liver transplantation), PTBD has the potential for technical difficulties. In addition, for new practitioners of this procedure, understanding the bile duct anatomy (especially the right hepatic bile duct) can be challenging. A procedure to drain bile to relieve pressure in the bile ducts caused by a blockage. An x-ray of the liver and bile ducts locates the blockage of bile flow. Images made by ultrasound guide placement of a stent (tube), which remains in the liver. Bile drains through the stent into the small intestine or into a collection bag outside the body. This procedure may relieve jaundice before surgery. Also called percutaneous transhepatic cholangiodrainage and PTCD.
CT-guided FNAC of small thoracic mass lesions (one cm or smaller) can provide high diagnostic accuracy rates approaching those of larger lesions. In cases of malignancy of the lungs, cyto-pathological examination of material obtained by CT-guided FNAC offers a quick and specific diagnosis which helps clinicians implement appropriate anticancer measures like chemotherapy and radiotherapy. It has also been demonstrated in literature that CT-guided FNAC is an accurate and sensitive way of diagnosing malignancy of the lungs.On the other hand, post procedure complications are fewer except for pneumothorax, pulmonary hemorrhage, and hemoptysis in a small percentage of cases. Severe chronic obstructive pulmonary disease, bleeding diathesis, and pulmonary arterial hypertension are the relative contraindications.